As a female plastic surgeon I do a lot of cosmetic breast surgery. My passion for breast surgery started early in my career when I began specializing in breast cancer reconstruction cases. Today, I perform over 250 cosmetic breast implant related cases every year, including primary breast augmentations, complex implant revisions, and increasingly more explant (or breast implant removal) surgeries.
Despite the common misconception, implants do not need to be replaced every 10 years. Medically speaking, the main reasons for implant removal are painful capsular contracture, implant rupture, or development of anaplastic lymphoma or squamous cell cancer around the implant. In reality though, women choose to remove their implants for many different reasons. Some are no longer happy with the size, shape or feel of breast implants. Other patients have concerns about how implants might be affecting their overall health.
So, what can you expect from explantation surgery?
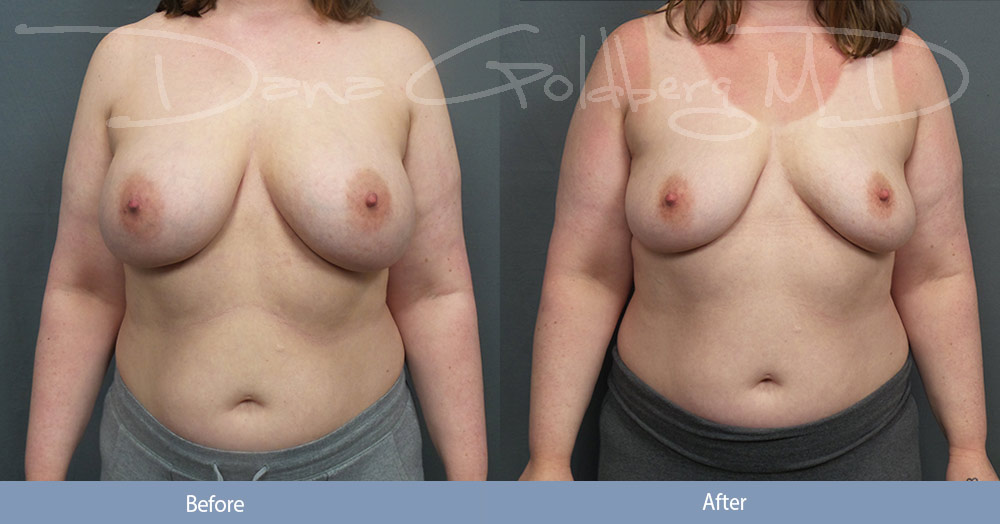
There has been a lot of attention in the past few years about the possible connection of breast implants with autoimmune disease or other systemic symptoms. This is also referred to as Silicone Incompatibility Syndrome (SIS), Autoimmune/Inflammatory Syndrome Induced by Adjuvants (ASIA), and Breast Implant Illness (BII). This is not a clinically recognized diagnosis because there are so many common symptoms that overlap with other causes and because no clear studies have identified (at least yet!) or identified criteria for a distinct illness caused by the presence of breast implants.
Recent studies presented to the American Society of Aesthetic Plastic Surgeons studied the relationship between breast implant removal and resolution of symptoms such as fatigue, joint aches, and other BIII symptoms. They also evaluated the amounts of heavy metals and bacterial DNA in the capsules and breast tissue as well as autoimmune lab work. The studies compared women with implants who had symptoms of BII and women with implants who did not have such symptoms. It also compared tissue samples from women who had never had implants. No specific connection was found between the amount of capsule removed and the resolution of symptoms. And no significant and consistent differences were found in lab work, infection rates, or heavy metal analysis. In fact, most of the heavy metals used during the implant manufacturing process that are concerning to patients are found in much higher concentrations in municipal drinking water.
Some surgeons promote (and some patients request) “En bloc” removal of their implant. This means that the implant and capsule are removed together in one piece. With thickened capsules from capsular contracture or when implants are placed above the muscle, the capsule can be very easy to separate from the breast tissue, and the only limit to removing the implant en bloc is the length of the incision. In other cases, the capsule is extremely thin (even see through) or very stuck to the surrounding bones and muscles. In these cases, trying to remove it can lead to an increased risk of bleeding, muscle damage, or lung injury. The only situation which requires removal of the implant and capsule en bloc is cancer within the capsule, which is extremely rare. For the vast majority of patients, total capsulectomy (removing the whole capsule, but not necessarily in one piece) or removing only part of the capsule is a safer alternative with less risk of complications and less risk of a poor cosmetic result.
A breast lift can be done at the same time as explant surgery, as can fat transfer to improve volume and shape. Adding additional procedures increases the cost of surgery, the time under anesthesia, and the risk of wound healing complications or tissue loss. This risk is higher for patients with thinning of the breast tissue from implants and patients with multiple scars from multiple surgeries.
Recovery:
A drain is placed on each side after surgery, which is removed about one week after surgery. Most patients are able to return to a light duty job at 4-7 days and a more physical job or exercise between 2 and 4 weeks after surgery.
Capsule vs Implant
No matter what the case, breast implants can safely whether it be removed En Bloc or not. If you are interested in learning more, please contact us.
Still want to learn more?
Watch these videos on our Facebook:
- Capsular Contracture. What is it? How does it happen and what you can do once it occurs?
- Wine Down Wednesday: Implant History & Safety
- Wine Down Wednesday: Breast Implants & ALCL
READ MORE ABOUT IMPLANT REMOVAL
- Are Breast Implants Safe?
- How Long Do Implants Last?
- Breast Implants & Cleavage
- What If I Have Cystic Breasts?
- How Until My Implants Feel Normal and Natural?
- Can I Breast Feed w/ Breast Implants?
- Can My Body Reject Breast Implants?
- Whats the Day of Breast Augmentation Surgery Like?
- Where Are Breast Implant Incisions Made?
- Will I Get Stretch Marks from Breast Augmentation?


